Movement Based Interventions – What Are Its Benefits?
Movement based interventions are of different types.
Research shows that multiple movement therapies can be used successfully for individuals with ASD but not every individual will experience the same benefits. Individuals with ASD are all different, creating a variety of positive and negative reactions to the different types of movement therapies.
But why are movement-based interventions important for this population?
-
It is a type of physical activity. “Children with ASD or other developmental disabilities who have limitations in physical activity are at risk for obesity and certain ASD medications have been shown to cause significant weight gain” (Fragala-Pinkham, Haley & O’Neil, 2011, MOVEMENT THERAPIES 3 p. 230)
-
It provides an avenue for social interaction, especially for children
-
Movement therapies can assist in improvements in the individuals’ three domains of learning (psychomotor, cognitive and affective), and contribute to an improved emotional state and leisure development (De Vries, Beck, Stacey, Winslow & Meines, 2015).
Let’s look at some research…
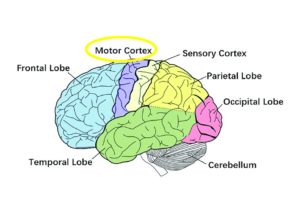
In a study done in 2005 by Oberman et. al(4), it was found that the motor cortex controls the “Mirror Neurons” which is involved in imitation, language, theory of mind and empathy; and deficits in these can cause social and communicative deficits in ASD.
In another study done in 2009 by Mostofsky et. al(5), the following findings were reported:
-
Decreased cerebellar activation resulted in difficulty in making motor movements more automatic.
-
Decreased connectivity between Cerebellum and Motor Cortex resulted in poor coordination in the development of automatic movements.
-
These reduced connectivities led to impairments in motor development and delayed acquisition of gestures important for socialization and communication.
Recent systematic investigations in 2011 by Mosconi, Takarae and Sweeney(6) indicated impairments in vestibular control, gross and fine motor movements, oculomotor functions and praxis in the majority of individuals with motor impairments and dyspraxia.
But why do we need to know all this?
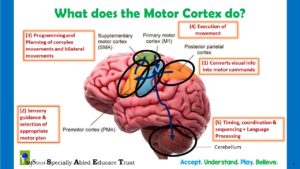
Because speech is purely a motor act! And is controlled by the motor cortex in the brain like all motor movements.
As you can see in the illustration above, the act of speech involves the following:
-
Converting visual information into motor commands
-
Sensory guidance and selection of appropriate motor plan
-
Programming and planning of the appropriate motor movements (complex and bilateral)
-
Execution of required motor movements
-
Appropriate timing, coordination and sequencing of the motor movements
-
Communication between left and right hemispheres of the brain to strengthen the corpus callosum.
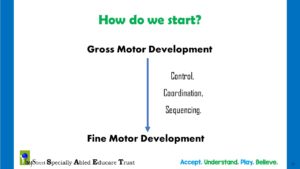 To create such a controlled, coordinated and sequenced act such as speech, we need to work not directly on speech alone but connect and strengthen the neuronal connections that enable gross motor skills… all the way to the fine motor skills.
To create such a controlled, coordinated and sequenced act such as speech, we need to work not directly on speech alone but connect and strengthen the neuronal connections that enable gross motor skills… all the way to the fine motor skills.
So, what are the movement based approaches that help a child develop the gross motor skills needed to develop controlled, coordinated and sequenced fine motor movements?
-
Sensory Integration
-
Gross motor activities (Motor Planning, Crossing-midline, etc.)
-
Yoga
-
Music and Movement (AMT, DMT)
-
Daily Routines/Chores (bathing, dressing, cooking, sweeping, watering plants, etc.)
-
Fine Motor activities
-
Oral Sensory and Motor activities targeting speech movements
-
AAC (Alternative and Augmentative Communication)

All the above-mentioned approaches will enable and develop motor patterns in the brain that will work towards developing controlled, coordinated and sequenced motor patterns for speech.

Why is it helpful to add music?
-
It’s fun for children!
-
When we listen to music, virtually the whole brain is involved.
-
Listening Programs enable neural symphony, connecting the various parts of the brain together.
-
Music and Language are processed by the same brain systems (Memorization and Rules of Language)
-
Music calms us and regulates us
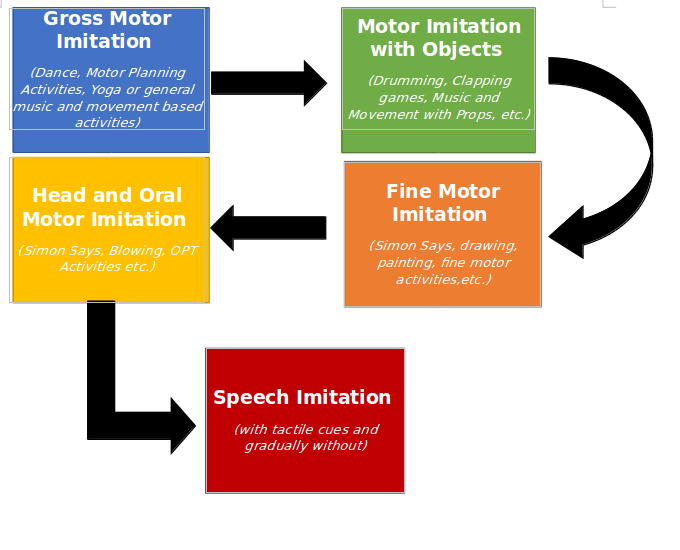
How can we work towards Speech Imitation?
References
(1) Bradish, Courtney, “Movement Therapy for School Age Children with Autism: A Review of the Literature” (2017). Kinesiology, Sport Studies, and Physical Education Synthesis Projects. 38.
-
https://digitalcommons.brockport.edu/pes_synthesis/38
(2) Fragala-Pinkham, M., Haley, S. & O’Neil, M. (2011). Group swimming and aquatic exercise programme for children with autism spectrum disorders: A pilot study. MOVEMENT THERAPIES 36. Developmental Neurorehabilitation, 14(4): 230-241. Doi:10.3109/17518423.2011.575438
(3) De Vries, D., Beck, T., Stacey, B., Winslow, K. & Meines, K. (2015). Music as a therapeutic intervention with autism: a systematic review of the literature. Therapeutic Recreation Journal. Retrieved December 10, 2017 from: https://www.highbeam.com/doc/1P3-3779575161.html
(4) EEG evidence for mirror neuron dysfunction in autism spectrum disorders. Lindsay M. Oberman, T, Edward M. Hubbard, Joseph P. McCleery, Eric L. Altschuler, Vilayanur S. Ramachandran, Jaime A. Pineda. Cognitive Brain Research 24 (2005) 190 – 198.
(5) Mostofsky SH1, Powell SK, Simmonds DJ, Goldberg MC, Caffo B, Pekar JJ. Decreased connectivity and cerebellar activity in autism during motor task performance. Brain. 2009 Sep;132(Pt 9):2413-25. doi: 10.1093/brain/awp088. Epub 2009 Apr 23.
(6) Mosconi MW, Takarae Y, Sweeney JA. Motor impairments and dyspraxia in autism. In: Amaral DG, Dawson G, Geschwind DH, editors. Autism Spectrum Disorders. New York: Oxford University Press; 2011. pp. 355–380



2 Comments
Padmini · January 12, 2021 at 11:52 am
This article is very informative.
Ashita Sengupta · October 23, 2021 at 11:11 am
Am looking for some guidance in speech therapy for my son from Shereen ma’am